What Is Photodynamic Therapy?
Selective destruction of cancer cells using a chlorophyll-based dye and laser light, with minimal side effects.
A light therapy that uses photosensitizing substances to specifically treat diseased tissue.
Photodynamic therapy (PDT) uses natural dyes together with light to gently destroy cancer cells. These dyes are called “photosensitizers” (PS) because they are taken up by cancer cells and make them sensitive to light of certain wavelengths.
Photodynamic therapy has a history of nearly 100 years and has been used successfully for a variety of tumors. Superficial tumors of the skin, lungs, intestines, and urinary bladder are particularly well suited because they are easily reached by the light. However, tumors in solid organs such as the kidney or prostate can also be treated with PDT.
How Does Photodynamic Therapy Work?
Free radicals activated by light attack the cancer cells and destroy them.
When a cancer cell that has absorbed the photosensitizer is exposed to light of a specific wavelength, the light energy triggers chemical reactions that generate reactive oxygen species. These oxygen compounds are highly toxic to cells and lead to tumor cell death.
In general, photosensitizers are initially taken up by all cells. However, the accumulation of PS in tumor cells is higher than in normal body cells, so that, depending on the type of PS, concentrations in cancer cells can be 10 to 20 times higher. Accordingly, when the tissue is irradiated with light, tumor cells primarily die off while normal cells survive.
Depending on the photosensitizer and type of treatment, PDT can also be used to selectively target tumor blood vessels through vascular-targeted photodynamic therapy, thereby reducing the blood supply required for tumor growth.
In addition, PDT triggers an immune response against the tumor cells because the dying tumor cells release tumor antigens that are recognized by the immune system. Similar to vaccinations, these tumor antigens enable the killer cells of the immune system to locate and destroy tumor cells in the body.
Call us now on +49 (0)177 23 82 863 or get in touch using the contact form
How is photodynamic therapy performed?
Light of a certain wavelength is the key.
PDT is a two-step process. First, the photosensitizer is administered, usually by intravenous infusion.
Three hours after administration, the PS has accumulated in cancer cells. By this time, the PS has already left normal cells through metabolic and transport processes.
In the second step, the cells are exposed to light of a specific wavelength that is absorbed by the PS. This activates the PS and destroys the cell. Because the PS accumulates selectively in cancer cells, the tumor is primarily destroyed while normal tissues and cells are spared.
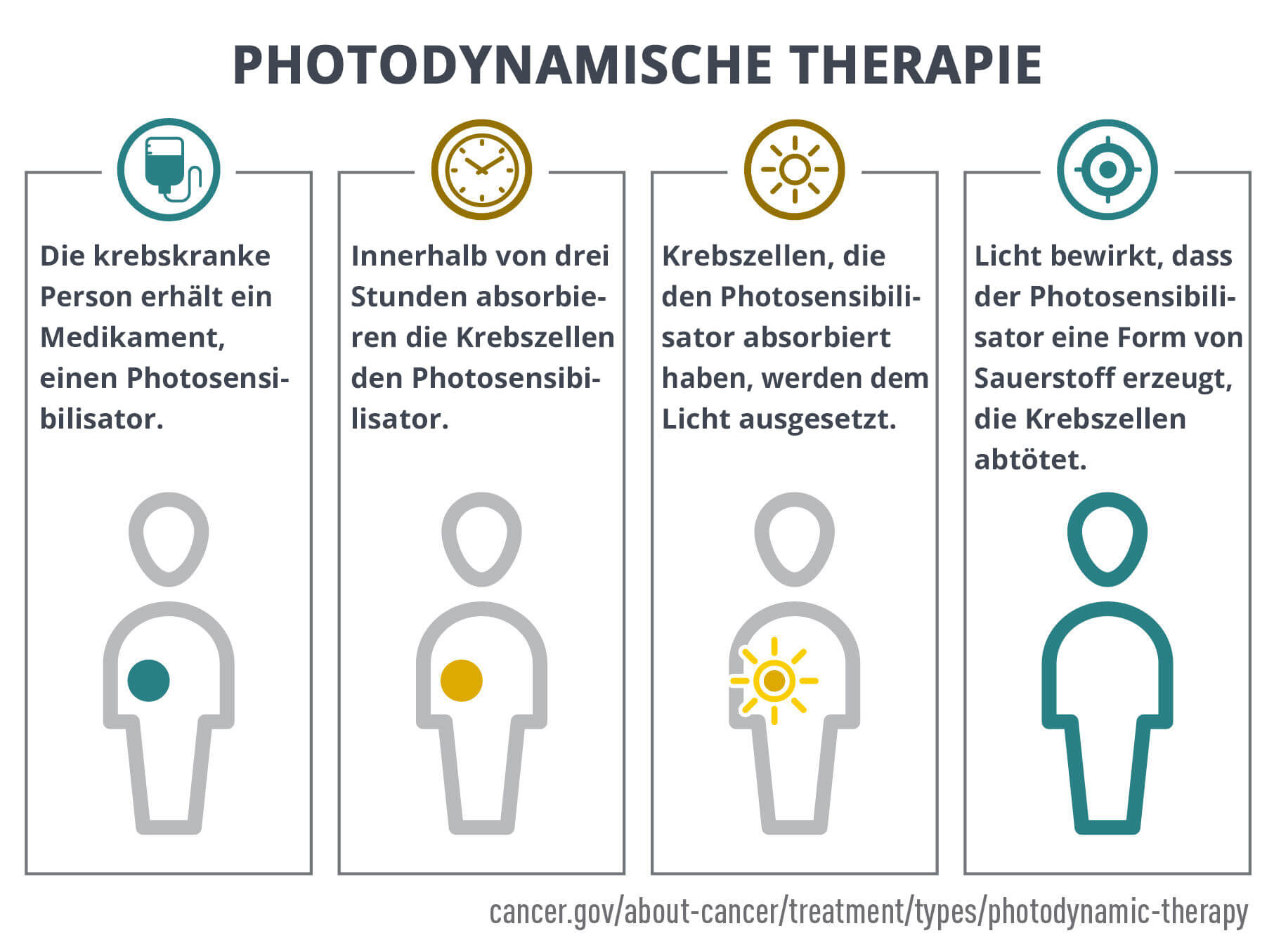

Advantages of photodynamic therapy
The gentle PDT procedure offers patients many advantages.
- PDT primarily destroys tumor cells and spares normal cells and tissue.
- In addition, PDT destroys cells without heating, unlike widely used thermal ablation techniques such as radiofrequency ablation (RF ablation) and High-Energy Focused Ultrasound (HiFU). As a result, PDT preserves the tissue structure of fibers and the interstitial matrix, as well as nerves and vessels.
- This enables functional preservation of anatomical structures. In the treatment of the prostate, this includes preserving erectile function by protecting the neurovascular bundle, a vascular and nerve plexus on the prostate that is destroyed during HiFU treatment or surgical removal of the prostate.
- The bladder sphincter can also be preserved during PDT treatment, even when there is partial infiltration by tumor tissue.
- PDT also minimizes scarring and induces strong secondary immune effects against cancer cells.
Potential side effects of photodynamic therapy
Although PDT is very gentle for the patient, some side effects can still occur.
Damage to normal cells from PDT, although limited, can cause burn-like symptoms, swelling, pain, and scarring in the treatment area. Other possible side effects, depending on the part of the body being treated, include:
- Cough
- Difficulty swallowing
- Stomach pain
- Pain when breathing
- Shortness of breath
- Skin problems such as redness, stinging, swelling, or itching
Chlorin E6, a photosensitizing drug, is used to mark cancer cells.
Photodynamic therapy with chlorin E6 for prostate cancer
In PDT of the prostate, light guides are inserted into the prostate at regular intervals through the pelvic floor, the perineum, using a stepper, an ultrasound transducer in the rectum, and a perforated plate (brachytherapy grid). The light guides are typically placed 1 cm apart, because the emitted laser light has a maximum penetration depth of about 2 cm. They can be inserted focally into the part of the prostate where the cancer is located or can cover the entire prostate if the tumor is extensive.
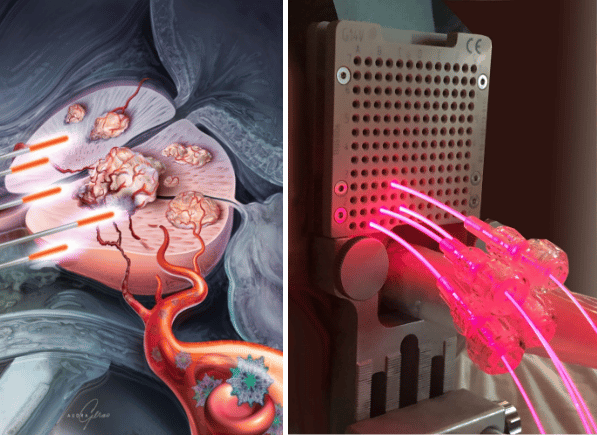
The photosensitizer Chlorin E6 is then injected into the patient as a short infusion. This photoactive substance is distributed throughout the body via the bloodstream but accumulates up to 20 times more in tumor tissue than in healthy cells. In Chlorin E6 photodynamic therapy for prostate cancer, the tumor cells are irradiated with monochromatic red laser light, which causes the cancer cells to die.
What is Chlorin E6 and how does it work?
When using Chlorin E6, healthy cells remain largely unaffected.
Chlorin E6 is a photosensitizer that specifically accumulates in tumor tissue. Green porphyrin is produced from plant material1. Chlorin E6 accumulates 20-fold more in tumor tissues than in healthy cells. If the tumor cells are irradiated (with monochromatic laser light with a wavelength of 665 nanometers – red light), the energy of the laser light is transferred to the chlorin E6 molecule.
The absorbed energy is transferred to oxygen molecules in the cell, creating oxygen radicals with highly reactive singular electrons. These oxygen radicals are highly reactive and react with biological components of the tumor cell such as the nucleus, mitochondria and cell membrane. As a result, the tumor cell loses its function and structure and dies.
Surrounding healthy cells that have not accumulated chlorin E6 remain largely unaffected by the red laser light.
The substance has already been successfully tested in a phase IIb clinical trial for the treatment of central bronchial carcinoma. In the available studies and experiences within the framework of healing trials, Chlorin E6 did not show any serious side effects.
Other photodynamic therapy methods for prostate cancer
The Tookad process
Another photodynamic therapy method for prostate cancer, the so-called Tookad method, has already been in clinical use for some time. In contrast to the photosensitizer Chlorin E6, the photosensitizer used in the Tookad procedure does not accumulate strongly selectively in tumor cells. In Tookad, irradiation with laser light primarily leads to a blockage of the blood vessels that supply the tumour. Tookad procedures therefore do not selectively kill off individual tumour cells, but rather cut off part of the prostate from the bloodstream.
For which prostate cancer patients is photodynamic therapy particularly suitable?
In contrast to surgical, chemotherapeutic, or radiotherapeutic procedures, PDT places a significantly lower burden on the patient.
Although there are no clinical studies to date that clearly indicate in which cases of prostate cancer photodynamic therapy is particularly suitable, it can be concluded from the lower side effect profile of PDT that it may be especially appropriate for treating localized prostate cancer when the patient wishes to avoid side effects such as impotence and incontinence.
PDT should also be considered and weighed against alternatives such as IRE or electrochemotherapy (ECT) for tumors that infiltrate critical structures such as the bladder sphincter or bladder floor.
PDT also represents a therapeutic alternative for patients who are considered “out of treatment” in the conventional medical sense or for patients who reject conventional therapies.
Other cancers and precancerous lesions treated with photodynamic therapy
In addition to the treatment of prostate cancer, PDT is also used for a number of other diseases.
The U.S. Food and Drug Administration (FDA) has cleared photodynamic therapy for the treatment of the following conditions:
- Actinic keratosis
- Advanced cutaneous T-cell lymphoma
- Barrett esophagus
- Basal cell carcinoma of the skin
- Esophageal Cancer
- Non-small cell lung cancer
- Squamous cell carcinoma of the skin (stage 0)
PDT is also used to relieve symptoms caused by the following cancers (palliative, not curative):
- Esophageal cancer when it blocks the esophagus
- Non-small cell lung cancer when it blocks the airways
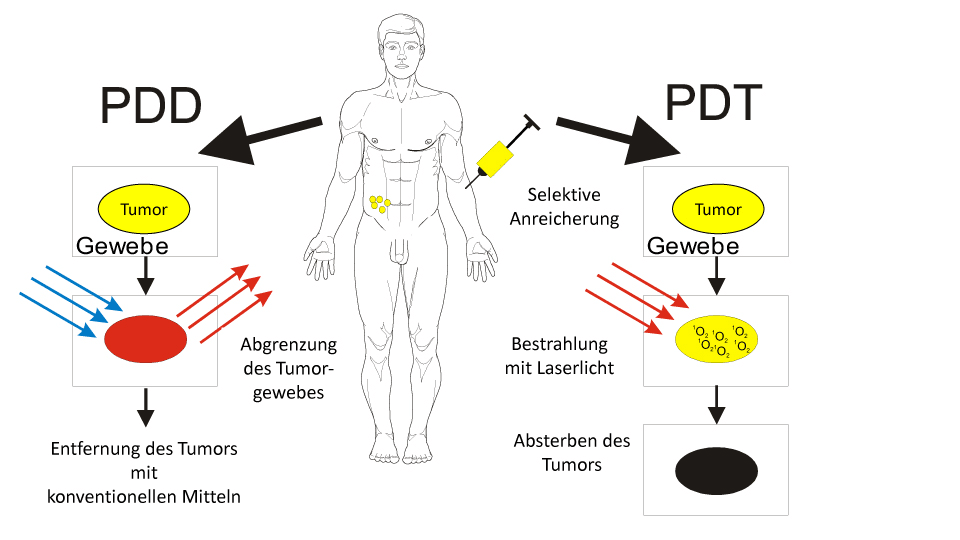
Photodynamic therapy (PDT) is also possible with Chlorin E6 (right side of the illustration). Three hours after the injection of Ce6, the tumor cells have taken up the substance. Irradiation with special laser light triggers a chemical reaction in the tumors that produces singlet oxygen.
Frequently Asked Questions
Yes, photodynamic therapy may be considered for selected prostate tumors. It targets prostate cancer cells that absorb higher amounts of the photosensitizer and respond to light activation. MRI imaging and clinical evaluation are used to determine whether PDT is appropriate for an individual case.
Recovery is usually quick because PDT is non-thermal and largely preserves surrounding tissue. Most patients return to normal daily activities within a few days. Temporary local effects such as swelling, urinary symptoms, or discomfort can occur as the treated tissue heals.
PDT is designed to spare nerves, vessels, and connective tissue by avoiding heat or surgical removal. This approach aims to preserve continence and erectile function whenever possible. Functional outcomes depend on tumor location and treatment extent.
PDT may be considered when a tumor is close to sensitive structures or when a patient prefers a non-thermal, minimally invasive approach. The choice between PDT, IRE, or ECT depends on tumor size, MRI findings, and individual treatment goals.
Photosensitizers can temporarily increase sensitivity to bright light. Patients are advised to avoid direct sunlight and strong indoor lighting for a short period after treatment. Your care team will provide specific guidance based on the photosensitizer used.

