Metastasis search – whole body staging
The search for metastases using CT and bone scintigraphy.
In the case of cancer, a distinction is made between the primary tumor, in the case of prostate cancer in the prostate gland, and possible sites of the primary tumor in other parts of the body, often in lymph nodes and bones, so-called metastases. Most deaths are caused by metastases.
The search for metastases is called “whole body staging.” To date, computed tomography (CT) and bone scintigraphy have been performed for this purpose in Germany. This is outdated! This is because CT can only detect the size of lymph nodes but not whether they are affected by prostate cancer. Bone scintigraphy, on the other hand, shows the frequent signs of wear and tear in the skeletal system, which are then mistaken for metastases.
PSMA PET/CT with gallium68
A modern and functional nuclear medicine imaging method.
Direct detection of metastases in prostate cancer is achieved by PSMA-PET1 – a functional nuclear imaging method. PSMA refers to the prostate-specific membrane antigen found on prostate cancer cells. In PSMA-PET, a ligand labeled with a gallium68 atom binds to PSMA receptors and visualizes prostate cancer metastases.
In Holland, PSMA-PET/CT has meanwhile replaced the old whole-body staging with bone scintigraphy and CT.
Talk to us on 069 50 50 00 980 or send us an e-mail using the contact form.
If whole-body staging with PSMA-PET – then do it right!
The new gold standard for finding metastases in prostate cancer.
PSMA-PET is also being performed more and more frequently in Germany. Unfortunately, often with poor technique, which can lead to unclear or even misleading results.
This results in part from the design of the PET scanners. First generation PET scanners produced only PET images. These are functionally valuable, but hardly represent the anatomy of the body. In the second generation, PET scanners were then combined with computed tomography (CT) scanners, resulting in mapping of function and anatomy. In combined PET/CT, however, CT is also used to make the PET images themselves better, through what is called “absorption correction.” In the third generation, only PET scanners are also combined with magnetic resonance imaging (MRI): PET/MRI. Touted as the non-plus-ultra, these provide worse results than second-generation PET/CT because no “absorption correction” is possible with MRI. However, the devices are popular because it is easier to bill for the exams.
Therefore, make sure that your PSMA PET is performed with optimal technique:
| CORRECT | FALSE | Justification |
| PSMA PET/CT PET and computed tomography | PSMA PET/MRI PET and magnetic resonance imaging | Only the combination of PET with CT allows a so-called “absorption correction”. PET and MRI is more lucrative for physicians but of poorer quality |
| Nuclide gallium68 (Ga68) | Nuclide fluorine18 (F18) | Reliable detection of the primary tumor and metastases in prostate cancer is only possible with the nuclide Ga68. A PSMA-PET with F18 often shows false positive results, nuclide enrichments that are not cancer foci. |
| Sufficient amount of nuclides, approx. 200 -250 MBq. | Too low nuclide quantity, 80 – 150 MBq | Since the nuclides are of short half-life, they quickly lose their effectiveness. Often, a dose is also divided for several patients. |
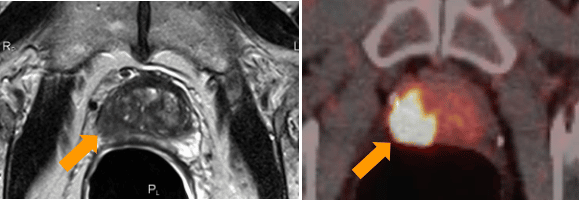
PSMA-PET/CT in the diagnosis of primary tumors
The combination of MRI and PSMA-PET can provide an accurate assessment of the aggressiveness of prostate cancer.
The use of PSMA-PET in the primary diagnosis of prostate cancer is becoming increasingly important. For example, if a cancer site is found in the MRI scan, the primary diagnostic test for the prostate, it may be possible to confirm the site using PSMA-PET, and a biopsy may not be necessary prior to treatment. Also, the combination of MRI and PSMA-PET may allow a more accurate assessment of the aggressiveness of prostate cancer than the Gleason score of the biopsy (scientific studies are currently being conducted on this). A biopsy can then be performed in the same session as the treatment, i.e. intraoperatively, instead of before the carcinoma is treated.
In Holland, PSMA-PET/CT has meanwhile replaced the old whole-body staging with bone scintigraphy and CT.